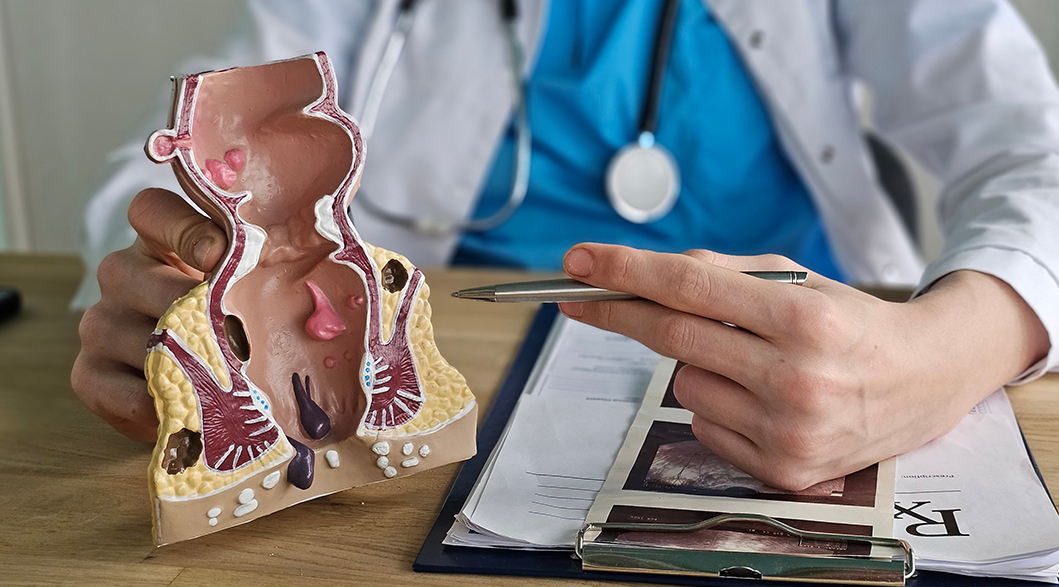
When you hear about colon polyps, you’d most likely associate them with cancer immediately. However, you may be relieved to know that this isn’t always the case. In fact, colon polyps are relatively common in adults over the age of 45, and the majority do not turn malignant.
These small growths develop on the lining of the colon or rectum and can vary in size and shape. As they often cause no early symptoms, colon polyps are frequently discovered incidentally during routine colonoscopy screening. While many never cause harm, certain types can gradually progress into colorectal cancer if left untreated, which is why doctors usually remove them when detected.
Understanding how colon polyps may present and when they require medical attention is an important part of early detection and prevention.
What Are the Symptoms of Colon Polyps?
One of the challenges with colon polyps is that they are often ‘silent’ or asymptomatic. Many people are unaware they have them until they are discovered during a routine screening. However, as polyps grow larger or if they become ulcerated, they may cause symptoms, including:
- Blood in your stool or rectal bleeding
- A persistent change in bowel habits (diarrhoea or constipation lasting more than a week)
- Unexplained weight loss
- Persistent abdominal pain
- Iron-deficiency anaemia
This makes it important to go for colonoscopies from age 50 or if you have otherwise been identified as a higher-risk patient.
What Causes Colon Polyps?
The exact cause of colon polyps is not always clear, but several factors are known to increase the likelihood of their development. Many of these factors influence how cells in the colon grow, repair and respond to inflammation over time.
- Age: The risk of developing colon polyps increases with age, particularly after 50, as cellular changes in the colon become more common.
- Family History: Having a parent, sibling or child with colon polyps or colorectal cancer may indicate that you are at a higher risk, due to a shared genetic or environmental influence.
- Genetic Conditions: Inherited syndromes such as Lynch syndrome or familial adenomatous polyposis (FAP) significantly increase the risk of polyp formation by affecting how colon cells regulate growth.
- Lifestyle Factors: Smoking and excessive alcohol consumption can damage the lining of the colon and promote abnormal cell growth.
- Excess Body Weight: Being overweight or obese is associated with higher levels of inflammation and metabolic changes that may encourage polyp development.
- Diet: Diets high in red and processed meats and low in fibre may also increase risk by affecting bowel function and prolonging contact between the colon lining and harmful substances.
- Inflammatory Conditions: Long-standing inflammatory diseases of the colon, such as ulcerative colitis or Crohn’s disease, can damage the bowel lining over time and increase the likelihood of polyp formation.
Common Types of Colon Polyps
Not all polyps are the same. When a polyp is removed, it is sent to a laboratory for analysis to determine its specific type. This classification helps your doctor understand the potential risk of cancer and decide how frequently you should have follow-up screenings.
Common types of colon polyps include:
Adenomatous Polyps (Adenomas)
Adenomas are considered pre-cancerous growths. Although they are not cancerous at the time of detection, they can develop into colon cancer if left untreated.
Hyperplastic Polyps
Hyperplastic polyps usually carry a very low risk of becoming cancerous. They tend to be small in size and are commonly found in the rectum or the sigmoid colon, which is the lower part of the colon.
Sessile Serrated Polyps
Sessile serrated polyps can be harder to detect because they are often flat and blend into the folds of the colon lining. Depending on their size and location, some of these polyps carry a higher risk of progressing to cancer.
Inflammatory Polyps
Inflammatory polyps are most often seen in people with inflammatory bowel disease, such as ulcerative colitis or Crohn’s disease. They form in response to ongoing inflammation in the colon and are generally non-cancerous.
How Are Colon Polyps Detected and Treated?
If you exhibit symptoms of colon polyps, your doctor may recommend screening options such as stool tests that check for hidden blood or DNA markers, or CT colonography, which provides a virtual scan of the bowel. However, if any of these tests suggest a potential issue, a standard colonoscopy is usually required to detect and treat these polyps.
Detection Via Colonoscopy
Colonoscopy remains the most effective method for detecting colon polyps, as it allows doctors to directly examine the lining of the colon and assess any abnormalities in real time. While the patient is under sedation, the doctor inserts a thin tube known as a colonoscope into the patient’s anus and uses a small camera in order to examine the area for abnormalities.
One of the major advantages of a colonoscopy is that it allows for both diagnosis and treatment in the same session. If your doctor finds a polyp, they will almost always move on to polypectomy.
Removal Via Polypectomy
Polyp removal, known as polypectomy, is carried out using the same colonoscope. A doctor can immediately begin this procedure by inserting specialised tools into the colonoscope that can be used to extract polyps.
Small polyps can often be removed with biopsy forceps. Larger polyps are usually removed using a wire loop called a snare, which may apply an electrical current to cut the polyp and seal the blood vessel at the same time. Since the lining of the colon does not contain pain-sensitive nerves, the removal process itself is painless.
Follow-Up After Polyp Removal
Once removed, the tissue is sent to a laboratory for analysis. The results will determine your future screening schedule. If only low-risk hyperplastic polyps were found, you may not need another exam for 10 years. However, if multiple adenomas, large polyps or serrated polyps were removed, your doctor might recommend a follow-up colonoscopy in 3 to 5 years to ensure no new polyps have developed.
Address Colon Polyps at Our Colorectal Screening Clinic
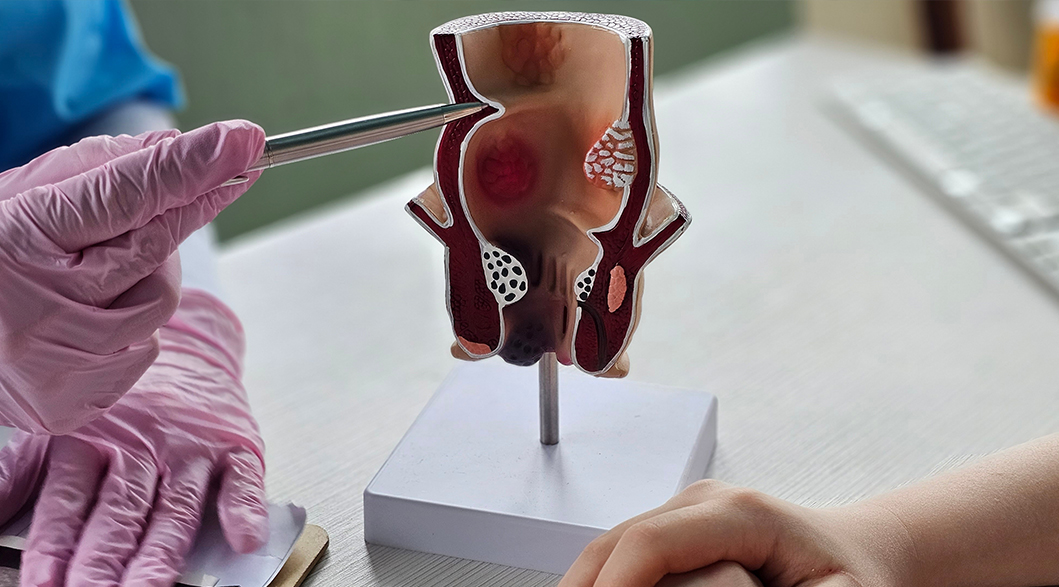
There is no guaranteed way to prevent colon polyps from developing. While lifestyle measures such as dietary changes and regular physical activity may support overall bowel health, their ability to prevent colon polyps varies between individuals and cannot be assured.
However, regular screening at a colorectal specialist clinic plays an important role in detecting and removing polyps before they have a chance to progress. Led by Dr Dennis Koh, Dr Sharon Koh Zhiling, and Dr Pauleon Tan Enjiu, our clinic offers comprehensive medical management for colorectal conditions.
If you are experiencing symptoms or are due for a routine screening, do not delay. Contact our clinic today to schedule a consultation with our experienced specialists. We are here to guide you through the process with care and expertise.



